|
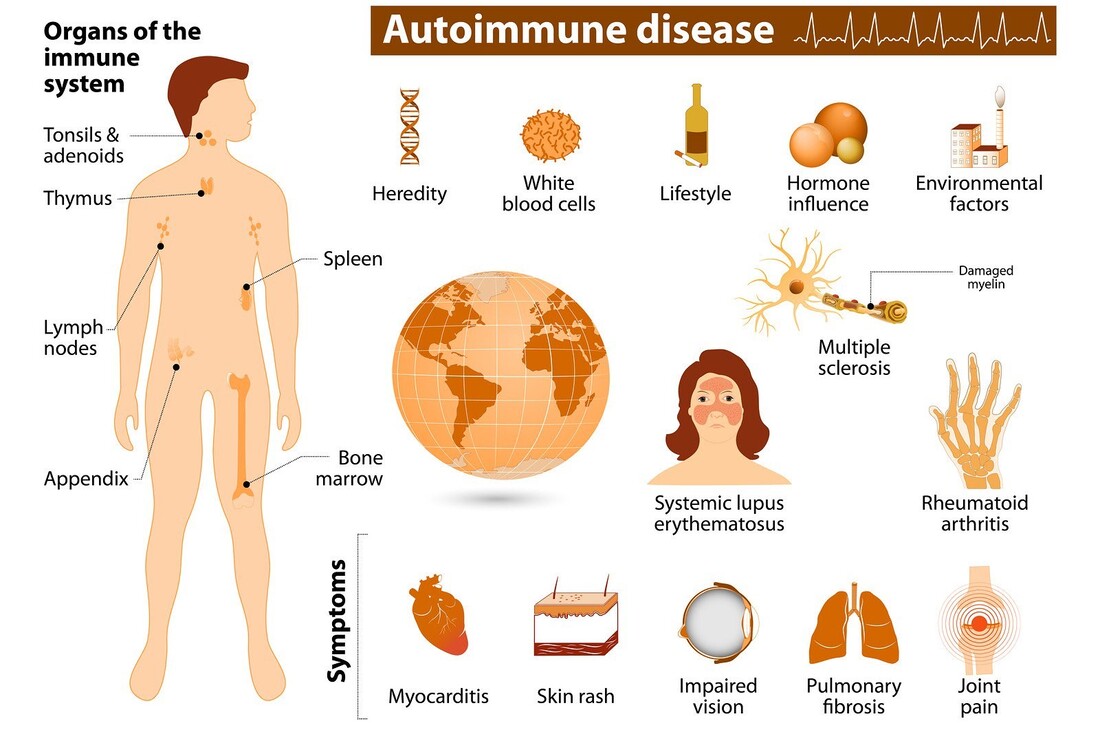
Image courtesy: Muhammad Zulfahmi (TBA6) Picture this: some people within your circle or maybe the closest one next to you right now may look as average Joe externally as you are. However, little do you know that one or a few of them are actually suffering internally. No, this is not a story of people who are struggling to move on after breaking up with their ex-partners. This is a story representing someone – who could be your neighbour, friend, relative, spouse or family member – struggling with an autoimmune disease, a permanent health condition. Now, what actually is an autoimmune disease? Have you ever heard of it? If you know anyone who is suffering from diabetes, type 1 to be specific, then you might know what an autoimmune disease is – only if the doctor tells you so. An autoimmune disease is basically a condition resulted from unusual immune response towards any functioning part of your body. The immune system fails to distinguish the body’s own cells or tissues and mistakenly attacks them assuming that they are invading the system. According to the United States (U.S.) Department of Health and Human Services, there are at least 80 types of autoimmune diseases ranging from the major organs, glands, digestive system and tissue. Among the common diseases that are considered as autoimmune diseases include celiac disease, Graves’ disease, rheumatoid arthritis, systematic lupus erythematosus (SLE), and inflammatory bowel disease (IBD). Medical records identified that the majority of patients who suffer from autoimmune diseases are women whom are often diagnosed as early as their adolescence and is much common during adulthood. An infographic summary of the autoimmune disease. - Image courtesy: National Institute of Environmental Health Sciences Causes and risk factors Despite being known since the early 1900s based on a research by Ananthanarayan and Paniker, the autoimmune diseases still have no definite root cause of what triggers them until today. Experts have only managed to come up with several theories of what factors lead up to the occurrence of autoimmune diseases such as genetic inheritance, hormonal status, virus or bacterial infection, environmental triggers, stress, smoking effects, and lack of nutrition. These risk factors are believed to encourage or further enhance the development of autoimmune diseases if not the exact cause. Symptoms The autoimmune diseases may vary in symptoms according to the type that one suffers from. Nevertheless, there are general symptoms of autoimmune diseases that most types share in common including fatigue, mild fever, loss of weight, rashes, muscle aches and joint pains, and even repetitive miscarriage in women. Such symptoms may fluctuate, it may occur for quite some time and then disappears before reappearing again later which is known in medical terms as a flare-up. In addition, there are also researches suggesting that autoimmune diseases may result into the build-up of cancer as one who suffers from an autoimmune disease have an increased chance of developing certain cancers. Autoimmune diseases causes inflammation on the affected area, which actually adds up to the risk of developing cancer. The IBD for instance, is most often associated with the development of colorectal cancer due to the severity of the inflammation in the gastrointestinal tract. Apart from that, SLE is also said to be linked with 16 types of cancer according to the data obtained from Arthritis Research & Therapy. Treatments Just like the symptoms, the treatments for autoimmune diseases vary depending on the type and also how severe the condition of the disease is. There is no permanent cure for autoimmune diseases though. Medications provided for autoimmune diseases are usually consumed lifelong to alleviate or control the disease in order to lessen the severity. This process is known in medical terms as remission. In general, among the types of medication often use to treat autoimmune diseases are anti-inflammatory drugs and glucocorticoids to reduce inflammation, blood transfusion for diseases that cause blood loss, vitamin or hormone supplements, and physical therapy. Even though the treatments help to relieve symptoms, patients on medication may experience side-effects from the medicines they consume. Personal experience As an autoimmune disease patient myself, I have been diagnosed with ulcerative colitis (UC), a form of IBD I suffered from about five years ago (2016). UC is a kind of IBD alongside Crohn’s disease, where it is a long-term condition that causes inflammation and ulcer in the colon and rectum. As said before, the cause is unknown and it happened so unconsciously. The very first symptom I could recall experiencing back then was when clearing my bowels, I noticed there were droplets of blood along with my stool. Since that it was the first time ever happened, I assumed that it was not so serious and that it would get well soon. I was wrong though. As days past, the bleeding in stool symptom continued. I resorted to a nearby clinic, I was only given some medicines but still have no clue of what it actually is since clinic doctors do not examine as detailed as hospital doctors. From days to weeks, and weeks to months, I started experience more symptoms overlapping with the first one. I started to easily feel nauseous which led to the loss of appetite, stools are no longer solid as they became softer – to the extent it became a watery diarrhoea, and I would frequently hit the toilet in a brief space of time due to the feeling of urgency. After discussing with my mother, we decided to consult a specialist at a local private hospital. An infographic about the two types of IBD: Ulcerative colitis and Crohn's disease. - Image courtesy: JAMA Network |
AuthorMuhammad Zulfahmi Bin Mohmad Fauzi ArchivesCategories |



 RSS Feed
RSS Feed
